Right now, much of America is reopening, thanks in large part to the COVID-19 vaccine rollout. Many states have eased restrictions and mask-wearing guidance from the Centers for Disease Control and Prevention (CDC) has relaxed for people who are vaccinated. But what does the data say about the progress in the fight against COVID-19 since the vaccine rollout started?
THE QUESTION
Has the daily death toll in the U.S. reached a pandemic low?
THE SOURCES
CDC data
Dr. Ali Mokdad, professor of health metrics sciences at the Institute for Health Metrics and Evaluation (IHME)
Dr. William Moss, executive director of the International Vaccine Access Center at Johns Hopkins Bloomberg School of Public Health
Dr. Saad Omer, director of Yale Institute for Global Health
THE ANSWER
The U.S. has not hit a pandemic low for daily COVID-19 deaths, though the current count is very close, and experts think the country will reach that milestone in the coming weeks.
WHAT WE FOUND
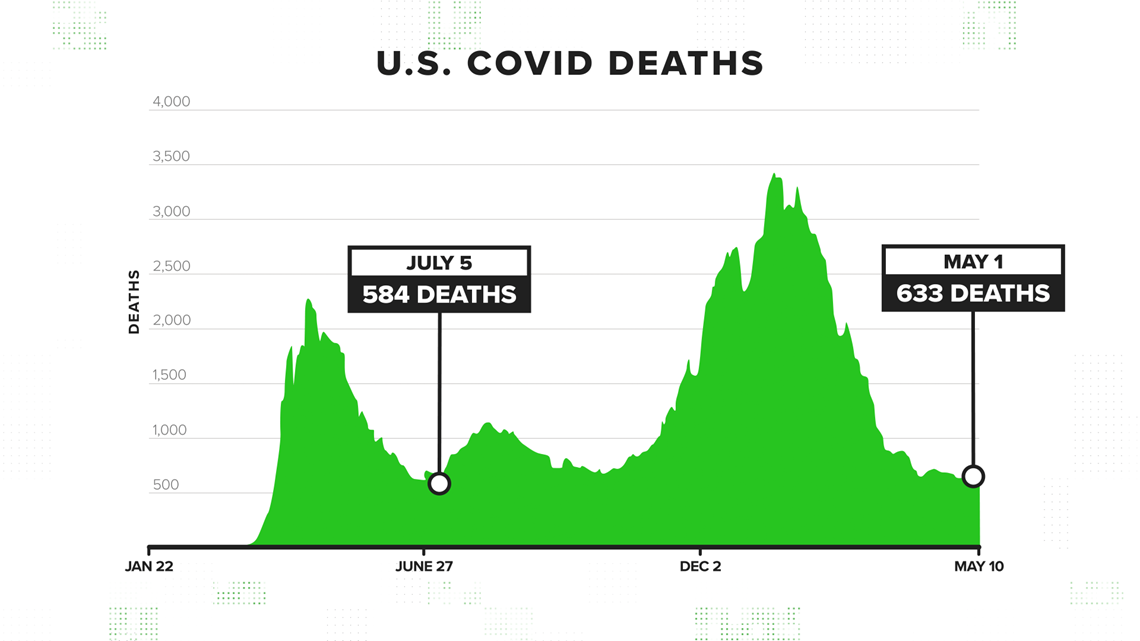
CDC data shows as of May 1, 2021, the average daily death count in the U.S. from COVID-19 (calculated from a 7-day total) was 633 deaths per day. That’s an 82% drop from the record-high death count last winter, which peaked on Jan. 13 with 3,427 deaths.
But it’s not the lowest total of the pandemic. For two days in July 2020, the average daily death toll dropped below 600 -- the lowest count was 584 deaths on July 5. That’s 8% lower than the May 1, 2021 total.

“We are coming down so fast right now, which is very good,” Dr. Ali Mokdad said. “I wouldn't say that we’re at the pandemic low... but we’re very close to it.”
Dr. Mokdad works with the Institute for Health Metrics and Evaluations (IHME), which produces COVID-19 data projections.
IHME is projecting the daily death count will drop another 80% between now and late summer, nearing 100 deaths per day in the U.S. by August.
“But never near zero simply because people are refusing to take the vaccine,” Dr. Mokdad said.
The death toll is dropping faster than the COVID-19 caseload, largely because more vulnerable populations are getting vaccinated.
CDC data shows that as of May 11, 35.1% of Americans were fully vaccinated. But 71.6% of people 65 and older were fully vaccinated, an age group that accounts for 80% of COVID-19 deaths in the U.S.
“Our main goal with our vaccination program is to reduce hospitalizations and deaths,” Dr. William Moss said. “We're not going to get it down to zero. Just like we don't get influenza virus deaths down to zero. But I think we can get it down to very low levels.”
Experts warn that progress could be at risk in the months ahead, especially with widespread vaccine hesitancy.
“One of the biggest threats is a variant that is less susceptible to our current vaccines,” Dr. Saad Omer said.
Dr. Omer fears that even as more Americans get their shots, pockets of unvaccinated people could experience COVID-19 flare ups in their communities. Those infections, along with outbreaks worldwide, like the one in India, increase the chances of the virus mutating into a dangerous variant.
“We as a world are letting this fire burn elsewhere,” Dr. Omer said. “And a widespread pandemic is a weird pandemic. It's a pandemic that has a high probability of newer variants emerging.”
Dr. Omer says, at this point, no existing variant is threatening the effectiveness of the vaccines.
“The current vaccines that we are using in the U.S. seem to be holding in terms of their high level of effectiveness,” Dr. Omer said. “But there is no certainty that will continue to be the case.”
Even without a dangerous variant, the team at the IHME is projecting a small surge in deaths next fall and winter.
“Because it’s a seasonal virus,” Dr. Mokdad said, arguing vaccines and masks will continue to be key to preventing a steeper spike. “We need to be vigilant.”
More from VERIFY: Yes, kids should get the COVID-19 vaccine
VERIFY
Our journalists work to separate fact from fiction so that you can understand what is true and false online. Please consider subscribing to our daily newsletter, text alerts and our YouTube channel. You can also follow us on Snapchat, Twitter, Instagram or Facebook.